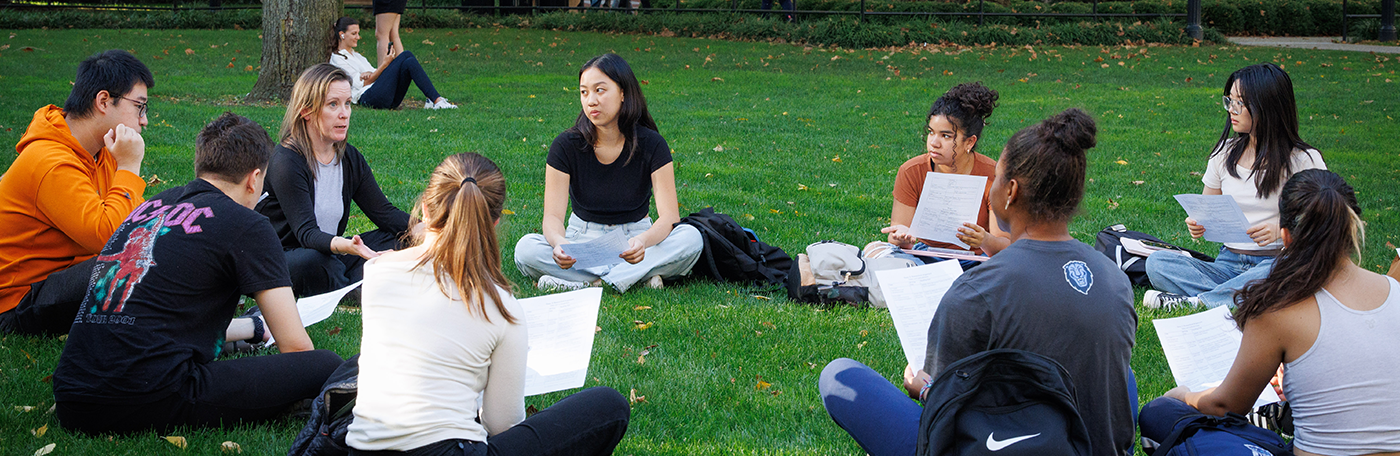Recent News from Columbia
Columbia Commits to Reducing Food-Related Carbon Emissions 25% by 2030
The University joins New York City mayor's office at Plant-Powered Carbon Challenge launch.
Statements From the April 17 Congressional Committee Hearing
Here are the full opening statements from Columbia representatives before the U.S. House Committee on Education and the Workforce.
A Statistician Shares the Best Things About Her Field
Tian Zheng, the Statistics department chair, is developing innovative tools to confront climate change and the opioid epidemic.
Research & Discovery
Arts & Humanities

Co-writer Ann Cooper’s Newshawks in Berlin describes the perils of reporting from war zones.

The GSAPP professor’s outdoor sculptures advocate for the experimental preservation of U.S. embassies.

In his new book, Dennis Yi Tenen presents AI as a matter of collaborative labor history.
Campus & Community
National & Global Affairs

The event convened leading policymakers, scholars, and advocates to discuss a range of issues, from reproductive rights to gender equity in the workplace to technology-facilitated gender-based violence.
Columbia in the News
Los Angeles Times, April 19
NBC News, April 18
Quanta Magazine, April 16