Prof. Kristin Myers Studies the Mechanics of Pregnancy
Kristin Myers was learning how to fix her father’s off-white Triumph TR4 roadster at the age of six. She later trained to be an automotive engineer and fully expected to have a career designing cars. But life takes unusual turns, and today, as an associate professor of mechanical engineering at Columbia Engineering, she is using her skills to examine the mechanics behind one of Mother Nature’s most important and little understood systems: pregnancy.

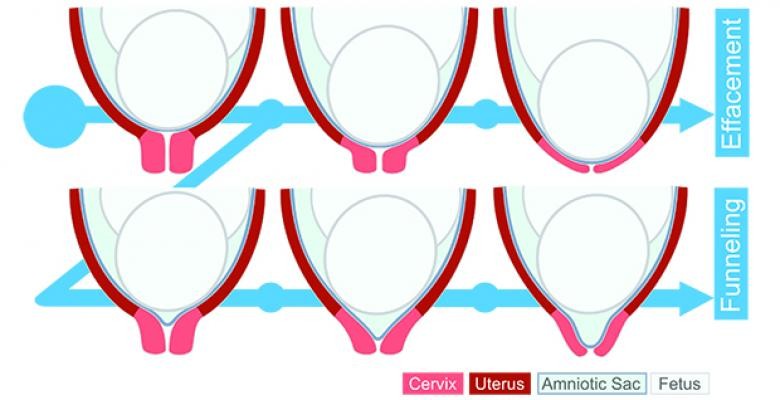
Myers studies the structures in the human body that facilitate childbirth, specifically the mechanical properties of the soft tissues involved in pregnancy—the cervix, the uterus and the amniotic sac— and how they interact and change over the course of gestation so that the body knows when it’s time to push a baby out into the world. She is also investigating how these mechanical miracles can go awry, leading to babies being born too soon.
Her research could have profound implications for the field of obstetrics and pediatrics, helping doctors better predict who is at risk of preterm birth (delivery before 37 weeks) and find better interventions for mother and child.
“All of the structural parameters in a woman’s reproductive organs play into how a baby will grow and occupy that intrauterine space,” she said. “Under all that pressure, how does the cervix stay shut? And in a brilliant reversal of roles, how does it open when it’s time to deliver the baby? These are the questions we want to answer.”
A native of Detroit, America’s automotive capital, Myers learned early about torque, force and other engineering basics from her father, an electrical engineer at Chrysler who raced cars in his spare time and took her to car shows. By the time she enrolled at the University of Michigan as a mechanical engineering major, Myers could take apart and rebuild a transmission. She spent four summers working at General Motors.
“I loved cars,” she says. “I still do. I grew up with everything mechanical. That basically explains who I am.” Then, in her junior year she took a research position studying the mechanical properties of natural rubber, whose strength and toughness is mysteriously greater than synthetic versions. “I loved the scientific aspect of the research, I realized I could apply my interest in engineering towards questions nobody had answered before.”
On a visit to MIT when she was applying to PhD programs, Myers learned of an intriguing new project studying the biomechanics of pregnancy. Once there, she combined her interest and training to tackle the mechanical properties of the cervix, which is located at the bottom of the uterus and keeps the fetus in the womb until it reaches full term. If it weakens and dilates prematurely, the result could be a miscarriage or premature birth.
The cervix softens throughout pregnancy, “an amazing mechanical feat in that it can go from something that’s very stiff to something that has to dilate to the size of a baby’s head.” she said. Myers obtained cervical samples from non-pregnant women to characterize the tissue in its normal state. She compared them to those from women who suffered from a rare condition that required them to undergo hysterectomies after a Caesarean section.
The pregnant sample was as elastic as a loose rubber band, and soft to the touch—it stretched but did not break. The normal tissue, by contrast, barely stretched at all.
What was it made of, Myers wondered? Once she came to Columbia in 2010, she pursued those questions with Joy Vink, an assistant professor of obstetrics and gynecology and a maternal fetal medicine specialist, and Christine Hendon, an associate professor of electrical engineering. It is believed the cervix is made mostly of collagen fibers, long proteins that may account for much of the tissue’s stiffness.
The Hendon lab used a technique called Optical Coherence Tomography to visualize how the collagen fibers of the cervix interweave, discovering that this tissue feature is responsible for the complex mechanical function of the cervix. The Vink lab expanded on this, showing that cervical muscle cells may form a sphincter whose function is to keep the uterus closed in pregnancy. Myers suspects the softening might be due to changes in the structure and organization of those collagen fibers, and is working on what could account for the mechanical changes.
Now, in collaboration with Columbia’s Department of Obstetrics and Gynecology, she is building a computer model of the cervix and related structures that will allow her to change variables and run simulations. As part of a five-year, $1.5 million NIH grant that began last September, she is using ultrasound exams to collect data on the anatomical changes of 50 women with normal pregnancies, measuring how much uterine, cervical and fetal membrane tissues stretch, grow and change.
Someday, she hopes, a pregnant woman will be able to visit her ob-gyn who will run an ultrasound and, based on a few variables and the expectant mother’s anatomy, predict exactly how her pregnancy is likely to unfold. “That is my Holy Grail,” Myers says.